Welcome to the Pharmacy Benefit Brief. This brief is your monthly snapshot of news from America’s prescription drug supply chain including pharmacy benefit managers, independent pharmacies, and drug manufacturers.
For Prescriptions It’s Home Sweet Home for Patients…

During the COVID-19 pandemic and long before, pharmacy benefit managers, PBMs, have provided home delivery of medications to help patients access needed prescription drugs safely, reliably, and conveniently. In fact, data show an increase in prescription drugs filled through mail-service pharmacy during the pandemic.
Unfortunately, state legislatures across the country are considering restrictions on PBMs’ ability to provide this vital service. Mail-service pharmacy should not be restricted as we continue to take precautions against the virus, and as we work to return to our normal way of life.
PBMs use sophisticated automation, geographically dispersed mail-service pharmacies, and technology to determine efficient delivery routes that help make home delivery of prescription drugs accurate, timely, and convenient. Additionally, they use temperature control packaging and notification of delivery for products that require it. Some groups, like pharmacists, are critical. of mail-service pharmacy because it takes consumers away from the pharmacy counter. That’s a red herring. If you’re worried about mail-service pharmacies’ ability to safely deliver medications – Don’t be.
Along with convenience, the benefits of mail-service pharmacy include higher rates of prescription adherence; 24/7 access to pharmacy counseling; improved health outcomes; cost savings from the use of generic drugs; greater dispensing accuracy; and, fewer medication errors (such as drug-to-drug interactions).
Learn the truth and visit “PBM Mail-Service Pharmacies.”
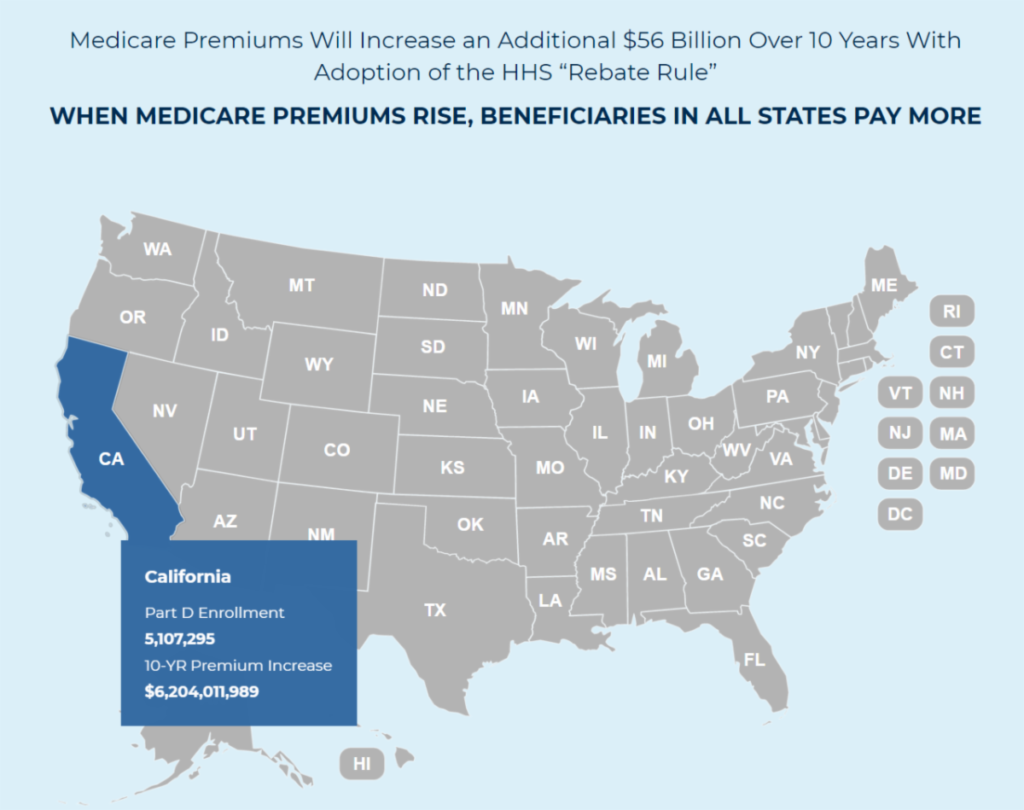
Impact of Rebate Rule on States…
The ill-advised, so-called “Rebate Rule” will significantly increase Medicare Part D’s premiums. To see how it would impact Medicare’s prescription drug benefits for beneficiaries in your state, please take a look at this interactive state-by-state map of Medicare Part D’s premium increases from the “Rebate Rule”: When Medicare Premiums Rise, Beneficiaries in all States Pay More.
Did you Know?
PBMs understand that for too many patients, prescription drugs can be unaffordable, particularly for patients in high-deductible health care plans. Recently, the IRS expanded preventive care benefits to include prescription drugs for patients with chronic conditions.
The federal guidance gives high-deductible health care plans, paired with health savings accounts, the option of allowing consumers to obtain medications, such as insulin, without paying cost sharing.
PBMs view this action as an important step forward in the fight to lower drug costs.
The Latest in Rx News
“PBMs are critical to the ability of Florida’s health plans to provide access to affordable, quality health care, which includes critical medications.” Those are the words of Audrey Brown, president & CEO of the Florida Association of Health Plans, Inc. Read more from Audrey in her op-ed: PBMs are a critical component of the health care supply chain.
Here’s an example of a pharmacist defending pharmacy benefit managers, PBMs. Mark N. Brueckl, assistant director of the Experiential Learning Program at the University of Maryland’s School of Pharmacy, has a commentary piece that’s worth a read: Pharmacy benefit managers are not to blame for high drug prices. The piece does a good job of explaining the PBM role with pharmacies and drug manufacturers.
“To the best of my knowledge, in the PBMs’ contracts with the pharmaceutical manufacturers, there are no requirements that manufacturers increase the prices of their drugs. The manufacturers do so to maintain or increase their profits.”

